Inflammatory Pain Treatment Options A Clear Practical Guide
Inflammatory pain treatment options
Inflammatory pain treatment options are often searched for when pain feels deep, persistent, warm, swollen, or flares without an obvious injury.
Inflammatory pain is driven by an active immune response inside the body, not simply wear and tear.
Understanding how this type of pain behaves helps you choose treatment options that calm inflammation rather than just masking symptoms.
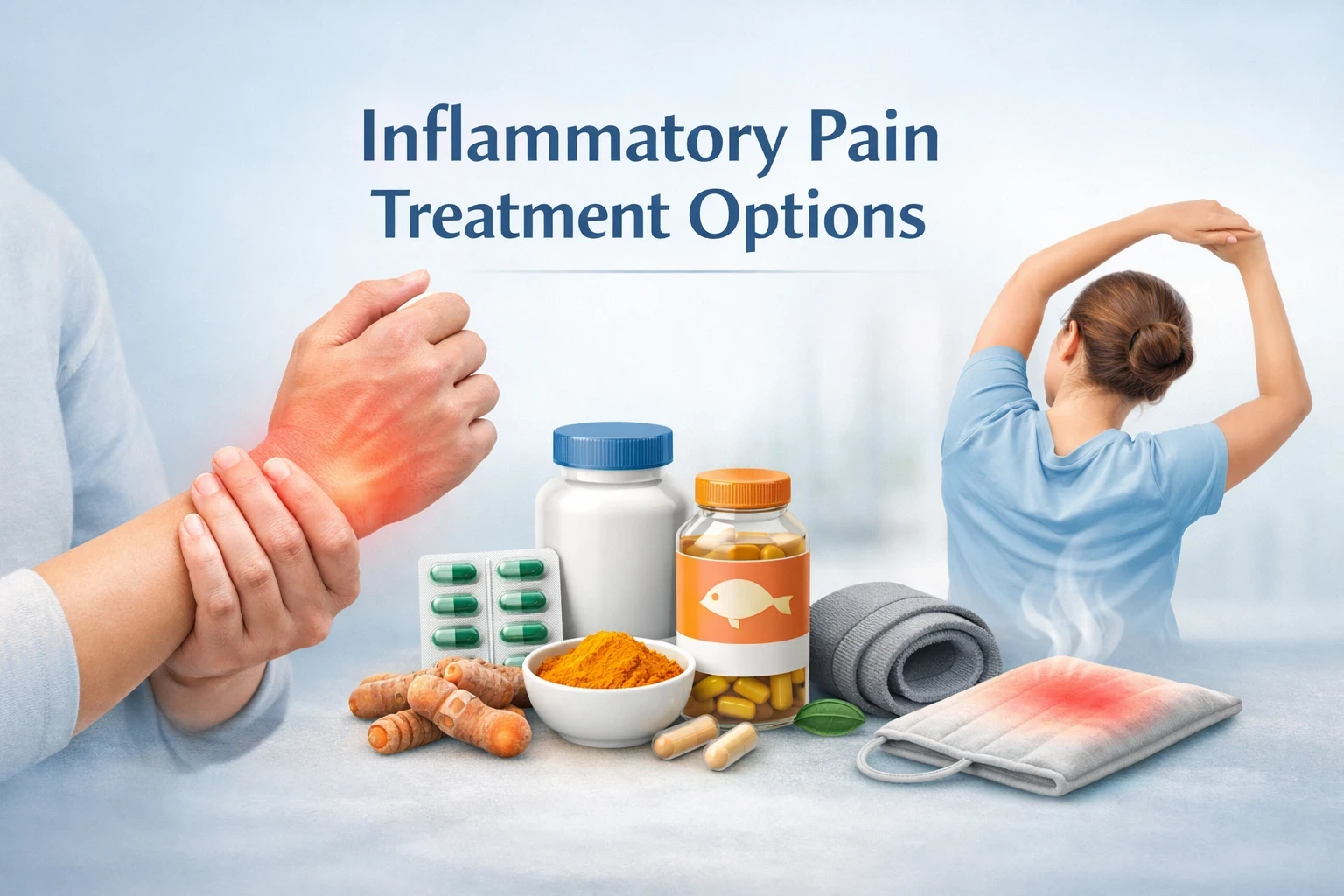
Inflammatory pain is common in conditions such as rheumatoid arthritis, inflammatory back pain, tendon flares, bursitis, and autoimmune-related joint pain.
It can come and go, feel worse in the morning, or flare after stress, illness, or poor sleep.
Treating inflammatory pain effectively usually requires a layered approach, not a single solution.
Understanding the Goal of Treatment
The goal of inflammatory pain treatment options is not just pain relief.
The real aim is to reduce inflammatory signaling, improve tissue tolerance, and calm the nervous system’s sensitivity to threat.
Pain intensity does not always equal tissue damage.
In inflammatory pain, the immune system stays switched on longer than needed, keeping tissues sensitive even when structural damage is minimal.
This is why treatment often works best when it addresses both biological inflammation and how the body processes pain.
For a deeper explanation of how long-lasting pain behaves, this overview can help:
👉 https://beyond-pain-relief.com/how-to-cope-with-chronic-pain/
Medical Treatment Options (Short-Term Support)
Medical inflammatory pain treatment options often include non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroids, or disease-modifying medications for autoimmune conditions.
These treatments can be helpful during severe flares or when inflammation threatens joint or tissue health.
However, long-term reliance may come with side effects, which is why many people explore supportive strategies alongside medical care.
Medication is often most effective when combined with movement, education, and lifestyle support rather than used alone.
Movement-Based Treatment Options
Gentle, consistent movement is one of the most effective inflammatory pain treatment options available.
Inflammatory pain tends to worsen with complete rest.
Light movement helps circulate inflammatory chemicals out of tissues and reassures the nervous system that movement is safe.
Effective options include:
- Walking at a comfortable pace
- Range-of-motion exercises
- Low-load strength work
- Swimming or water-based movement
The key is consistency over intensity. Small amounts done regularly outperform aggressive exercise that triggers flares.
Pain Education as Treatment
Pain education is a powerful but often overlooked inflammatory pain treatment option.
Understanding that pain can be amplified by the nervous system — not just damaged tissue — reduces fear and tension. This alone can lower pain intensity.
Learning how pain works helps people move with more confidence and less guarding, which gradually reduces inflammatory flare patterns.
This resource explains how education can directly reduce pain sensitivity:
👉 https://beyond-pain-relief.com/

Inflammatory Pain Treatment Options
Daily habits quietly influence inflammation levels more than most people realize.
Sleep disruption, chronic stress, and irregular routines increase inflammatory signaling.
Improving these areas does not eliminate pain overnight, but it often reduces flare frequency and intensity over time.
Helpful lifestyle options include:
- Consistent sleep and wake times
- Stress-regulation practices (breathing, time outdoors, pacing)
- Balanced nutrition with adequate protein and micronutrients
Reducing long periods of static postures
These changes support the body’s natural anti-inflammatory processes.
Ergonomics and Load Management
Poor workstation setup can silently worsen inflammatory pain, especially in the neck, shoulders, hips, and lower back.
Ergonomic adjustments are practical inflammatory pain treatment options because they reduce unnecessary tissue stress throughout the day.
This guide explains what actually matters when choosing supportive seating:
👉 https://beyond-pain-relief.com/ergonomic-office-chairs-for-back-pain-relief/
Reducing sustained strain allows inflamed tissues time to settle rather than being re-irritated daily.
Supportive Tools and Modalities
Some people benefit from temporary supportive tools as part of their inflammatory pain treatment options.
Examples include:
- Heat or contrast therapy
- Braces used briefly during flares
- Compression supports
Gentle self-massage tools
These do not cure inflammation but can reduce pain enough to allow movement and activity, which supports recovery.
The key is temporary use, not dependence.

Nutrition and Supplement Considerations
Nutrition influences inflammation, although it is rarely a standalone solution.
Commonly explored options include:
Magnesium for muscle and nervous system support
Responses vary widely.
Supplements work best when combined with movement, sleep improvement, and stress regulation rather than used in isolation.
Why One-Size-Fits-All Doesn’t Work
Inflammatory pain treatment options must be individualized.
What helps one person may flare another.
Autoimmune conditions, injury history, stress load, and sleep quality all influence how inflammation behaves.
Tracking patterns — not just pain levels — helps identify what supports recovery versus what quietly worsens symptoms.
Progress is usually non-linear, with good days and flares along the way.
Putting It All Together
The most effective inflammatory pain treatment options combine:
- Appropriate medical care when needed
- Gentle, regular movement
- Pain education
- Lifestyle support
Load and stress management
This layered approach reduces reliance on any single intervention and builds long-term resilience rather than short-term relief only.
Scientific Research
https://pubmed.ncbi.nlm.nih.gov/32679976

 Previous Post
Previous Post Next Post
Next Post