Fibromyalgia Pain Explanation Starts With One Important Truth:
Fibromyalgia Pain Explanation
Fibromyalgia pain explanation starts with one important truth: the pain is real, but it does not come from damaged tissues in the way most people expect. Instead, it involves how the nervous system processes signals.
Fibromyalgia is considered a central sensitivity condition. That means the brain and spinal cord become more reactive.
Signals that would normally feel mild can feel intense.
Over time, this heightened sensitivity can lead to widespread discomfort, fatigue, and sleep disruption.
Understanding what is happening beneath the surface can reduce fear and help people make practical decisions about managing symptoms.
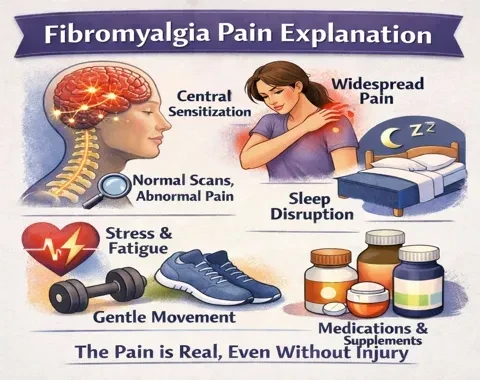
What Is Fibromyalgia?
Fibromyalgia is a long-term condition marked by widespread musculoskeletal pain, tenderness, fatigue, and cognitive symptoms often called “fibro fog.” It affects both men and women, though it is more commonly diagnosed in women.
If you want a deeper overview of symptoms and patterns, see this detailed guide on fibromyalgia pain symptoms: widespread and confusing.
Importantly, scans and blood tests usually look normal.
That can be frustrating. However, normal imaging does not mean nothing is happening.
It simply means the issue lies in pain processing rather than structural injury.
The Science Behind Central Sensitization
A proper fibromyalgia pain explanation must include central sensitization.
In simple terms, the nervous system becomes overly efficient at detecting and amplifying danger signals.
Think of it as a volume knob that has been turned up too high. Even light pressure or mild movement can feel painful.
Research shows that people with fibromyalgia often have:
• Increased levels of certain neurotransmitters involved in pain
• Reduced natural pain-inhibiting chemicals
• Heightened brain activity in pain-processing regions
Over time, this can create a cycle where poor sleep, stress, and inactivity further increase sensitivity.
If you’re exploring broader management strategies, you may find practical insights in treatment options for fibromyalgia pain.
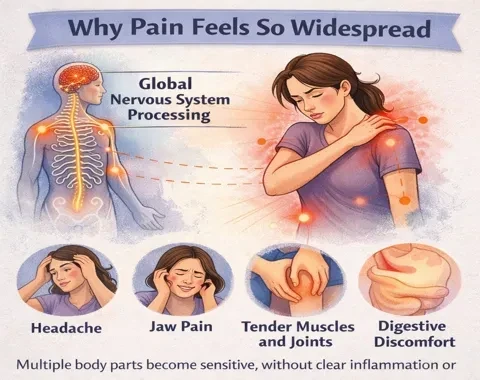
Why Pain Feels So Widespread
Unlike localized injuries, fibromyalgia pain is often described as aching, burning, throbbing, or stabbing across multiple areas of the body.
This widespread nature happens because the nervous system processes signals globally.
Muscles, joints, and soft tissues may feel tender even without inflammation or visible damage.
Many people also experience:
• Morning stiffness
• Heightened sensitivity to touch
• Headaches
• Jaw pain
• Digestive discomfort
The body can feel like it is constantly “on alert.”
The Role of Sleep and Fatigue
Sleep disruption plays a huge role in fibromyalgia.
Deep sleep is when the body restores tissues and recalibrates pain signals. When sleep is fragmented, sensitivity increases.
That is why sleep support is often a foundation of recovery strategies.
You can explore supportive ideas in what helps with fibromyalgia sleep problems.
Fatigue in fibromyalgia is not ordinary tiredness.
It can feel overwhelming and persistent, even after rest. This exhaustion further reduces resilience to pain.
Stress, Emotions, and the Nervous System
A balanced fibromyalgia pain explanation also includes stress physiology.
The nervous system is deeply connected to emotional processing.
Chronic stress can increase cortisol imbalance and sympathetic nervous system activity.
Over time, this keeps the body in a heightened state.
This does not mean the pain is psychological. It means the brain and body are closely linked.
Practical approaches such as pacing, gentle movement, breathwork, and stress management can gradually lower overall sensitivity.
Movement: Gentle but Consistent
It may seem counterintuitive, but total rest often makes fibromyalgia worse.
Gradual, low-impact movement helps retrain the nervous system.
Walking, swimming, light resistance training, and stretching can improve circulation and reduce stiffness.
For supportive products that may help ease daily strain, see fibromyalgia pain relief products: what helps and what to expect.
The key is pacing. Overdoing activity can cause flare-ups. Small, consistent steps are far more effective than sudden bursts of intensity.

Medication and Supplement Considerations
Doctors sometimes prescribe medications that influence neurotransmitters involved in pain signaling.
These medications could include nerve-modulating drugs oranti-depressants.
Some people also explore magnesium, vitamin D, or omega-3 supplements.
While supplements are not cures, correcting deficiencies may support overall nervous system function.
For the best quality assured supplements go to HerbsPro.
You should in the first instance consult a healthcare professional.
Flare-Ups: Why They Happen
Flare-ups often occur after:
• Poor sleep
• Emotional stress
• Illness
• Overexertion
• Weather changes
The nervous system becomes temporarily more reactive.
Recognizing triggers can help reduce the intensity and duration of flares.
Tracking patterns in a journal can be surprisingly helpful.
A Balanced Perspective
Fibromyalgia is complex. It is not caused by weakness, laziness, or imagination.
It reflects a sensitized nervous system that has become overly protective.
The encouraging news is that the nervous system can change.
Neuroplasticity works both ways.
With consistent habits, many people see meaningful improvement in pain levels and quality of life.
Progress is often gradual rather than dramatic. However, small gains add up over time.
Scientific Studies
https://pubmed.ncbi.nlm.nih.gov/18636094/
https://pubmed.ncbi.nlm.nih.gov/20638153/
https://pubmed.ncbi.nlm.nih.gov/31297168/
